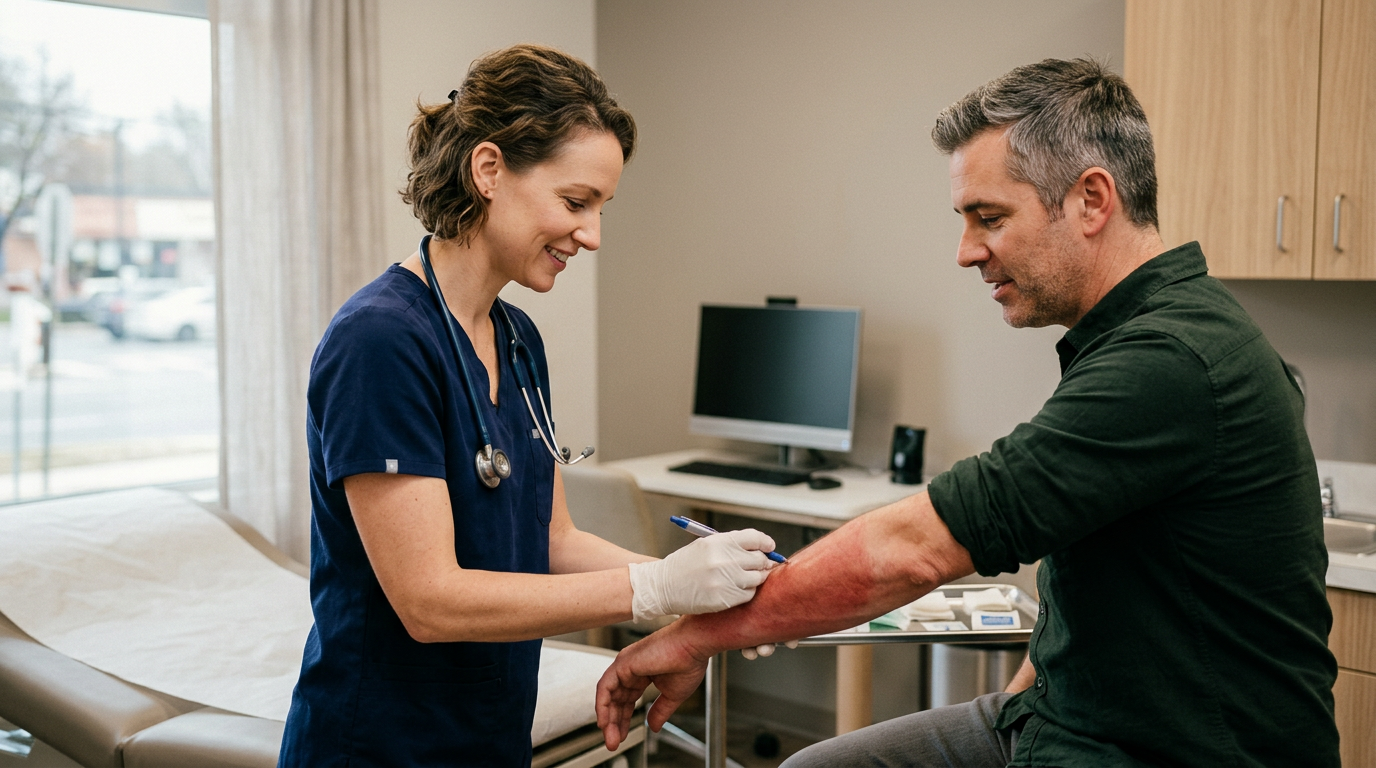
Urgent Care Tick Bite: When to Get Checked and What to Expect
You just found a tick embedded in your skin after a hike through the East Bay hills. Now you’re wondering: do I need medical attention, or can I just pull it off and move on? If you’re searching for urgent care tick bite guidance, here’s the short answer — most tick bites don’t cause illness, but some absolutely require prompt medical care. Therefore, knowing the difference could save you weeks of illness.
Medically reviewed by Sean Parkin, PA, CEO & Founder — Urgent Care
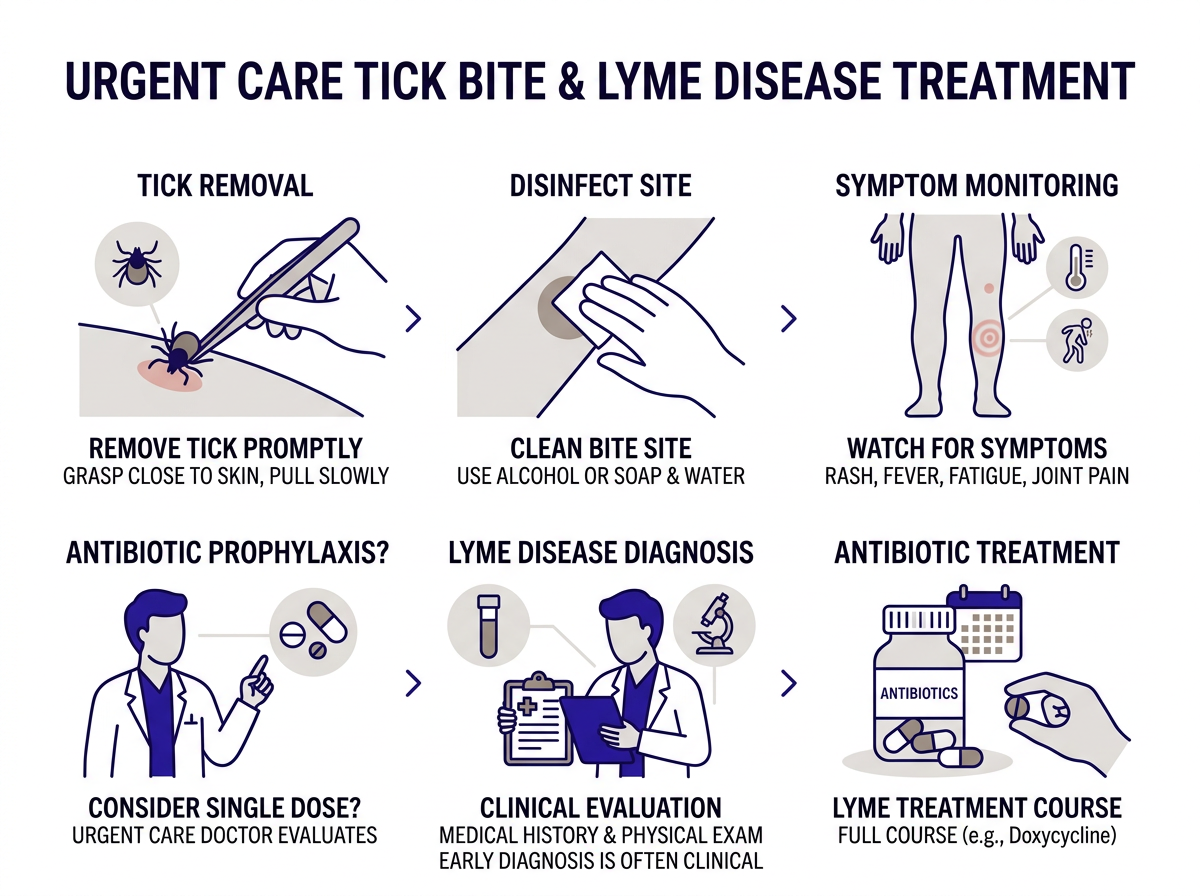
How to Remove a Tick Safely
Before you do anything else, get the tick off your body the right way. Because a botched removal can increase your risk of infection, take 60 seconds to do this properly.
Tools and Technique
What you need: Fine-tipped tweezers (not the wide, flat kind you use for eyebrows). If you don’t have tweezers handy, a tick removal tool works too.
Step-by-step removal:
- First, grasp the tick as close to your skin’s surface as possible. You want to grab the head, not the body.
- Next, pull upward with steady, even pressure. Don’t twist, jerk, or squeeze the tick’s body — this can cause the mouthparts to break off in your skin or push infected fluids into the bite.
- If the mouthparts remain in the skin, try to remove them with tweezers. However, if you can’t get them easily, leave them alone and let the skin heal.
- Then, clean the bite area thoroughly with rubbing alcohol, iodine, or soap and water.
- Finally, dispose of the tick by flushing it down the toilet, sealing it in tape, or placing it in a sealed bag with alcohol. Don’t crush it with your fingers.
Common Mistakes to Avoid
What NOT to do: Forget the folk remedies. Coating the tick in nail polish, petroleum jelly, or holding a hot match to it doesn’t work. In fact, these methods can cause the tick to burrow deeper or regurgitate bacteria into your bloodstream. According to the CDC’s tick bite guidelines, the only recommended removal method is steady upward traction with fine-tipped tweezers.
Pro tip: Also, save the tick if you can. Place it in a sealed plastic bag or tape it to an index card with the date written on it. If you develop symptoms later, identifying the tick species helps your provider determine the right treatment. For instance, some people even photograph the tick next to a coin for scale.
Will Urgent Care Do Anything for a Tick Bite?
Yes — and sometimes what urgent care does after an urgent care tick bite visit can prevent a serious illness before it starts. Specifically, here’s what happens during a typical visit.
Assessment. The provider will examine the bite site, ask when you found the tick, how long it was likely attached, and where you were when you picked it up. These details matter because transmission risk depends on the tick species and how long it was feeding.
Tick identification. If you saved the tick (or a photo), the provider can often identify the species. Blacklegged ticks (deer ticks) carry Lyme disease and are the primary concern in many parts of the country. In contrast, dog ticks carry Rocky Mountain spotted fever but not Lyme. Additionally, Western blacklegged ticks are present in Northern California, so Bay Area residents should be particularly aware.
Preventive antibiotics. This is the big one. If a blacklegged tick was attached for 36 hours or more, current guidelines recommend a single dose of doxycycline (200 mg) to prevent Lyme disease. However, this preventive treatment is most effective when given within 72 hours of tick removal. Consequently, getting to urgent care quickly after finding an engorged tick can make a real difference.
Wound care. If the bite area looks irritated or infected, the provider will clean it and may prescribe antibiotics for a secondary skin infection — separate from Lyme prevention.
Blood work. Urgent care won’t typically order Lyme disease blood tests at the initial visit. Why? Because it takes several weeks for antibodies to show up. As a result, testing too early almost always produces a false negative. However, if you develop symptoms later, urgent care can order blood work at that point.
How Soon After a Tick Bite Should You See a Doctor?
Timing depends on the situation. Here’s a practical breakdown:
Within 72 hours — if the tick was engorged (swollen, grayish) or you know it was attached for more than 24-36 hours. This window is when preventive antibiotics are most effective. So don’t wait for symptoms; the whole point is to prevent them.
Within 3-30 days — if you develop any symptoms after a tick bite (more on those below). Lyme disease symptoms can appear anywhere in this window, and earlier treatment leads to better outcomes. Since symptoms can be vague at first, err on the side of getting checked.
Immediately — if you develop a rapidly expanding red rash, high fever, severe headache, or muscle paralysis. These are signs of a serious tick-borne illness that needs prompt treatment.
For a straightforward tick bite where the tick was small, flat (not engorged), and easily removed, you can generally monitor at home. However, seeing a provider the same day is always reasonable if you’re uncertain. After all, peace of mind has value, and a quick evaluation is low-cost and low-risk.
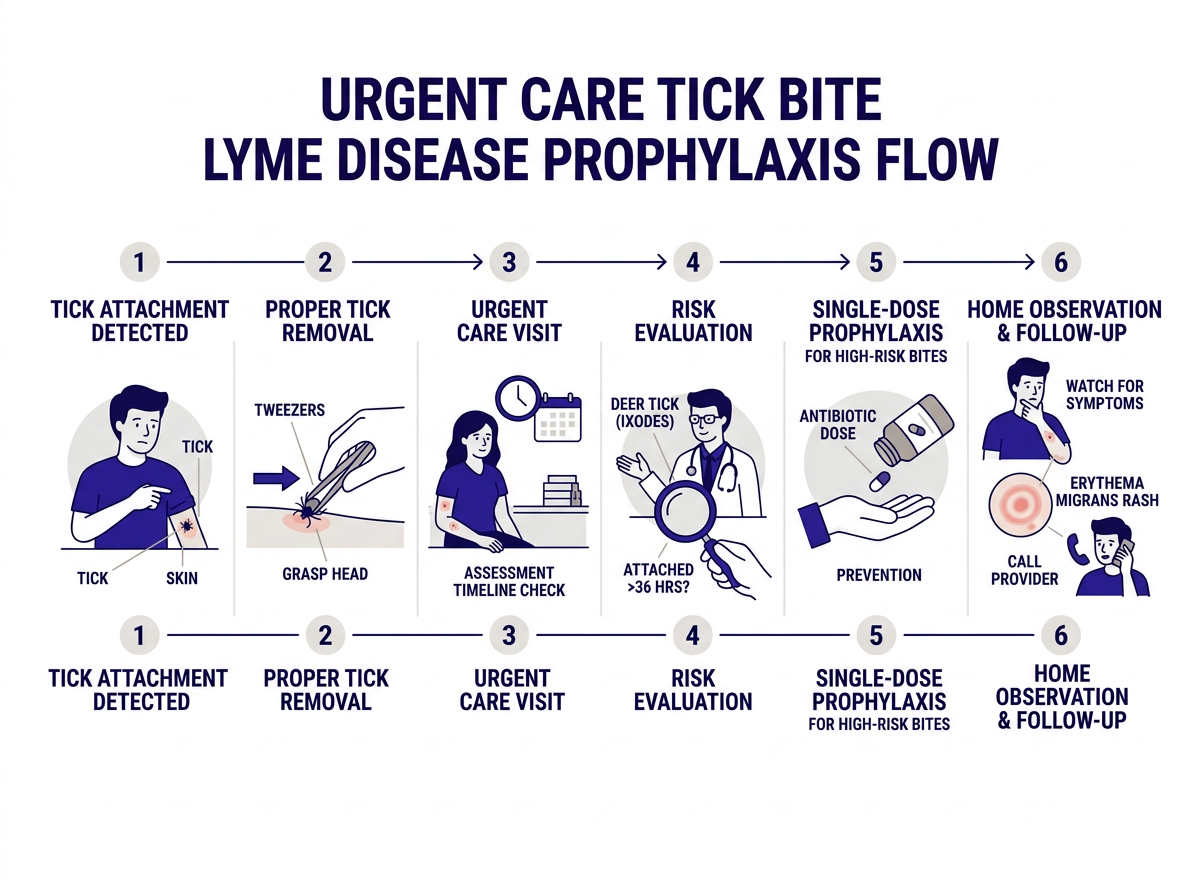
What Are the Early Signs of Lyme Disease?
Lyme disease is caused by the bacterium Borrelia burgdorferi, transmitted through the bite of infected blacklegged ticks. If preventive antibiotics weren’t given — or if the infection takes hold anyway — these are the warning signs to watch for:
The Bullseye Rash and Other Symptoms
The bullseye rash (erythema migrans). This is the most recognizable symptom. It appears at the bite site as a red area that expands over days or weeks, often clearing in the center to create a target or bullseye pattern. It typically shows up 3-30 days after the bite and can grow to 12 inches or more across. Importantly, however, not everyone with Lyme disease gets this rash — roughly 20-30% of infected people never develop it. Therefore, the absence of a bullseye rash doesn’t rule out Lyme.
Flu-like symptoms. Fever, chills, fatigue, body aches, headache, and swollen lymph nodes — but without the respiratory symptoms you’d expect from an actual flu. If you feel like you have the flu in the middle of summer and you had a recent tick bite, then Lyme disease should be on your radar.
Joint pain. This is particularly common in the knees. Notably, Lyme-related joint pain can come and go and may affect different joints at different times.
Neurological symptoms. In later stages, untreated Lyme can cause facial palsy (drooping on one side of the face), numbness or tingling in the hands and feet, and also severe headaches with neck stiffness. These symptoms indicate the infection has spread beyond the initial bite site.
If you notice any of these symptoms after a tick bite, don’t chalk it up to coincidence. Instead, visit urgent care and mention the tick bite — even if it happened weeks ago. Early-stage Lyme disease responds well to a 2-3 week course of oral antibiotics. In contrast, late-stage Lyme is harder to treat and can cause lasting problems.
How Can You Tell If a Tick Bite Is Serious?
Most tick bites cause nothing more than a small red bump that fades in a day or two. That’s a normal skin reaction, similar to a mosquito bite. However, a serious tick bite looks different.
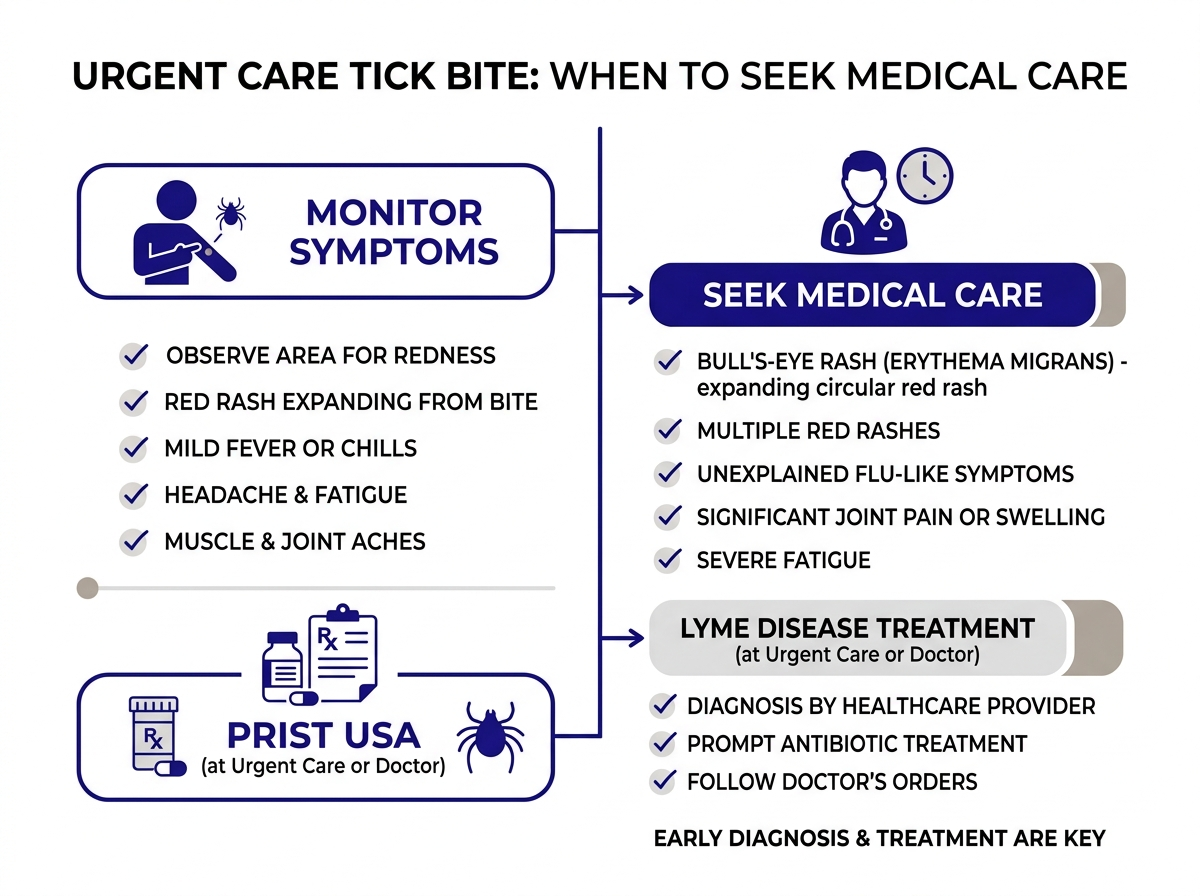
Signs the bite needs medical attention:
- A rash that expands beyond the initial bump, especially if it develops a ring or bullseye pattern
- Redness, warmth, or streaking spreading outward from the bite — signs of a skin infection
- Fever developing within days to weeks after the bite
- Unusual fatigue, headaches, or muscle aches you can’t explain
- Multiple rashes appearing on different parts of the body (a sign of disseminated Lyme)
- The bite area becoming increasingly painful rather than improving
Also consider the context. Were you in a wooded, grassy, or brushy area? Was the tick attached for a long time? Was the tick engorged (full of blood, appearing gray or swollen)? If so, an engorged tick has been feeding longer, which increases the chance of disease transmission. Similarly, the geographic location matters — Lyme disease is most common in the Northeast and upper Midwest, but Western blacklegged ticks in California can also carry the bacteria.
Preventing Tick Bites in the First Place
The best urgent care tick bite visit is the one you never need. If you spend time outdoors in the Bay Area — hiking in Redwood Regional Park, walking trails in Tilden, or even gardening in a leafy backyard — then these prevention steps are worth the effort.
- First, wear permethrin-treated clothing when hiking in grassy or wooded areas. Permethrin kills ticks on contact and remains effective through several washes.
- Also, use DEET or picaridin repellent on exposed skin. Products with 20-30% DEET provide several hours of protection.
- Additionally, do a full-body tick check after being outdoors. Check warm, hidden areas: behind ears, along the hairline, underarms, groin, behind knees, and around the waist. Ticks are small — nymphs are specifically the size of a poppy seed.
- Shower within two hours of coming indoors. Because ticks that haven’t attached yet can be washed off, this is a simple but effective step.
- Furthermore, tumble dry clothes on high heat for 10 minutes after outdoor activities. Heat kills ticks; washing alone may not.
- Finally, check pets too. Dogs and cats can carry ticks indoors on their fur. Run your hands over their coat after outdoor time, paying particular attention to ears, neck, and between toes.
Spring and summer are peak tick season in Northern California, although ticks can be active year-round in mild climates. Because of this, Bay Area residents should stay vigilant even outside the traditional “tick season.”
What to Do After an Urgent Care Tick Bite Visit
After your visit, follow these steps to stay on top of things:
- First, take any prescribed medication as directed. If you received preventive doxycycline, take it with a full glass of water and avoid lying down for 30 minutes afterward because it can cause esophageal irritation.
- Next, mark the bite site. Draw a circle around the redness with a pen so you can track whether it’s expanding. Also, take a photo daily for comparison.
- Then, monitor for 30 days. Set a reminder on your phone. If symptoms develop within this window, return to urgent care or see your primary care provider. Specifically, mention the tick bite history.
- Finally, watch for other tick-borne illnesses. Lyme disease gets the most attention, but ticks can also transmit anaplasmosis, babesiosis, and ehrlichiosis. Since symptoms overlap (fever, fatigue, aches), report any post-bite illness to a provider.
If you develop concerning symptoms weeks later, urgent care can refer you to a specialist — typically an infectious disease doctor — for more advanced testing and treatment.
Get Checked at CityHealth Urgent Care
Found a tick and not sure what to do? CityHealth Urgent Care in San Leandro can evaluate your bite, identify the tick if you saved it, prescribe preventive antibiotics when appropriate, and set you up with a monitoring plan. No appointment needed — just walk in during our hours or call (510) 984-2489. Learn more at cityhealth.com/urgent-care.