Hand Foot and Mouth Disease Treatment: A Parent’s Complete Guide
Your toddler woke up with a fever, won’t eat breakfast, and you just noticed tiny blisters on their palms. If you’re searching for hand foot and mouth disease treatment, here’s the good news: most cases resolve at home within 7 to 10 days without prescription medication. However, those 7 days can feel brutal for both kids and parents. This guide covers what works, what doesn’t, and when to head to urgent care.
Medically reviewed by Susana Quezada, NP — Nurse Practitioner
What Is Hand Foot and Mouth Disease?
HFMD is a viral infection caused by coxsackievirus A16 or enterovirus 71. It spreads through saliva, blister fluid, nasal secretions, and stool. As a result, children under 5 get it most often, although adults catch it too.
Symptoms typically show up 3 to 6 days after exposure. In most cases, they start with a fever between 101 and 103°F, followed by painful sores inside the mouth and a rash with small blisters on the hands, feet, and sometimes the buttocks or legs.
Because the virus spreads so easily, it tears through daycares and preschools fast. According to the CDC, HFMD is most contagious during the first week of illness. Moreover, the virus can live in stool for weeks after symptoms clear.
Hand Foot and Mouth Disease Treatment at Home
There’s no antiviral or antibiotic for HFMD. Instead, treatment focuses entirely on managing symptoms while the virus runs its course. For this reason, the following steps make the biggest difference in your child’s comfort.

Pain and Fever Relief
- Acetaminophen (Tylenol) or ibuprofen (Advil/Motrin) reduces fever and mouth pain. Follow dosing instructions based on your child’s weight.
- Never give aspirin to children, because aspirin during a viral illness can trigger Reye’s syndrome.
- For children over 6, a warm saltwater gargle (half teaspoon of salt in 8 ounces of warm water) can also soothe throat and mouth sores.
Keep Them Hydrated
Mouth sores make swallowing painful, so kids often refuse to drink. Consequently, dehydration is the number one complication risk with HFMD.
- Cold fluids work best. For example, water, milk, and diluted electrolyte drinks (like Pedialyte) go down easier when cold.
- Popsicles, frozen fruit bars, and ice chips numb the mouth slightly and provide hydration at the same time.
- Avoid acidic drinks. In particular, orange juice, lemonade, and soda burn open mouth sores. Similarly, tomato-based foods cause stinging.
Food That Won’t Hurt
Stick to soft, bland, cold foods during the worst of the mouth sores (usually days 2 through 5). For instance, try these options:
- Yogurt and smoothies
- Applesauce and mashed bananas
- Ice cream or frozen yogurt
- Lukewarm soup (not hot) and mashed potatoes
- Scrambled eggs
On the other hand, skip anything spicy, salty, crunchy, or acidic until the sores heal completely.
Skin and Blister Care
Don’t pop the blisters. The fluid inside is contagious, and popping them also increases infection risk. Instead, let blisters dry and crust over on their own.
In addition, keep the rash clean with gentle soap and water. If your child scratches at blisters, trim their nails short and consider lightweight cotton gloves at bedtime.
Day-by-Day HFMD Timeline
Understanding the progression of hand foot and mouth disease treatment helps you plan ahead and avoid unnecessary ER trips. Here’s what to expect:
- Days 1-2: Fever hits first (101-103°F). Your child may seem tired, cranky, and lose their appetite. Meanwhile, mouth sores begin forming.
- Days 2-4: Mouth sores peak, so eating and drinking become painful. At this point, blisters appear on hands, feet, and possibly buttocks. However, fever often breaks during this phase.
- Days 4-7: Blisters start crusting over. As a result, mouth pain improves and appetite returns gradually.
- Days 7-10: Most symptoms resolve. Nevertheless, skin may peel on the hands and feet for another week or two. Some children lose fingernails or toenails weeks later (this looks alarming but is harmless and temporary).
When to Go to Urgent Care for Hand Foot and Mouth Disease
Most HFMD cases resolve at home. However, certain signs mean your child needs a medical evaluation right away. Take your child to urgent care if you notice any of the following:
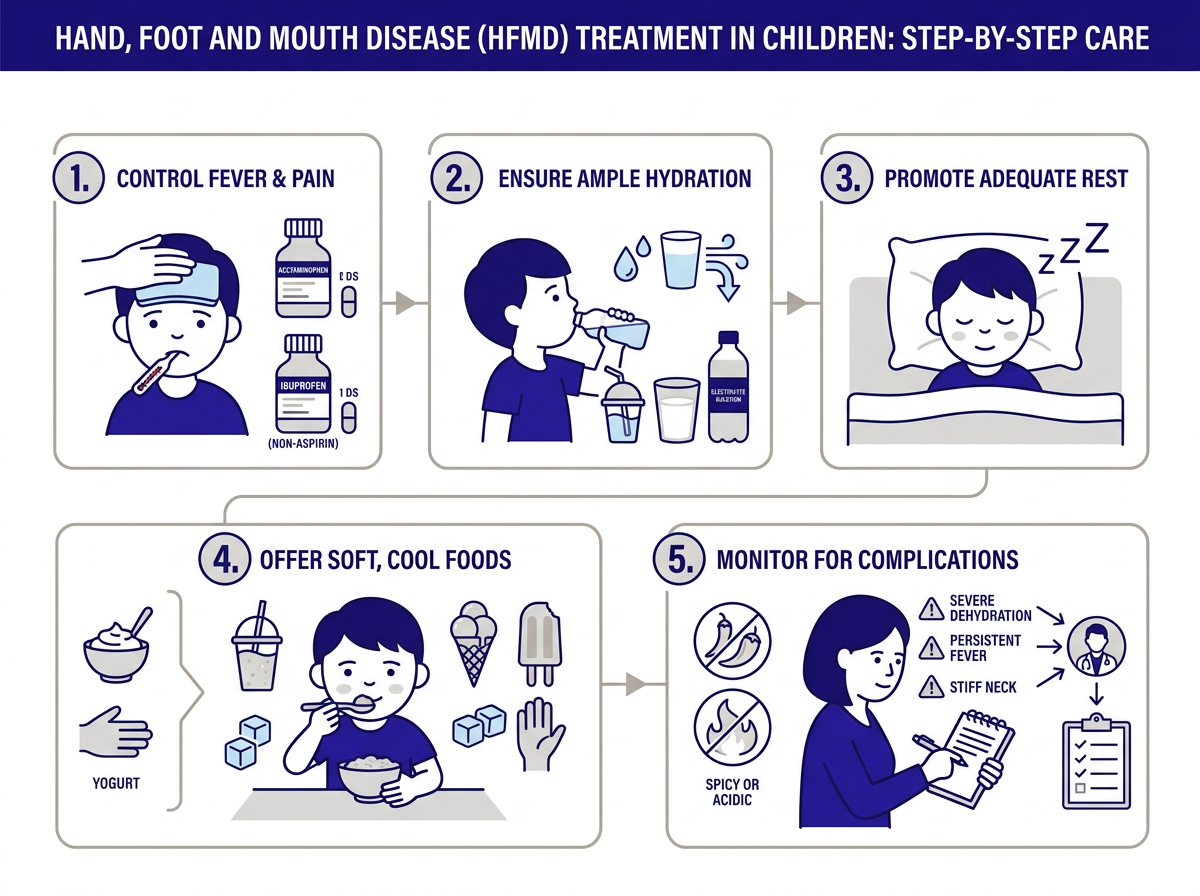
- Signs of dehydration: no wet diaper in 6+ hours, no tears when crying, dry lips, sunken eyes, or extreme lethargy
- Fever above 104°F or fever lasting more than 3 days
- Severe mouth pain preventing all drinking for more than 12 hours
- Symptoms getting worse after day 5 instead of improving
- Redness, swelling, or pus around blisters, because these are signs of secondary bacterial infection
- Stiff neck, severe headache, or confusion, which in rare cases can indicate viral meningitis
At CityHealth Urgent Care in San Leandro, we evaluate HFMD cases regularly, especially during spring and summer outbreaks. Walk in for same-day evaluation with no appointment needed.
HFMD in Adults
Adults often assume they’re immune, but that’s a misconception. In fact, parents catching HFMD from their kids is common, and adult symptoms can actually be more severe.
Adult hand foot and mouth disease treatment follows the same approach. Specifically, it involves:
- Painful mouth sores (often worse than in children)
- A rash on hands and feet that may blister or just feel tender
- Body aches and fatigue lasting up to 2 weeks
- Peeling skin on palms and soles several weeks after recovery
If your throat pain is severe enough that you can’t swallow fluids, visit urgent care for evaluation rather than waiting it out.
How Long Is HFMD Contagious?
HFMD spreads most aggressively during the first week of illness, especially before the rash appears. In other words, your child may be spreading it before you even know they’re sick.

Furthermore, the virus can persist in stool for several weeks after symptoms resolve, according to the Mayo Clinic. Therefore, strict hand hygiene after diaper changes matters long after your child looks healthy.
Daycare and School Return
Most childcare facilities require all three of the following before return:
- Fever-free for 24 hours (without medication)
- Mouth sores healed or nearly healed
- All blisters crusted over
Check your specific program’s policy, since some require a doctor’s note. CityHealth can provide return-to-school clearance during any walk-in visit.
Preventing Hand Foot and Mouth Disease
There’s no vaccine for HFMD. As a result, prevention comes down to hygiene basics:
- Wash hands frequently with soap and water for at least 20 seconds, especially after diaper changes and before eating
- Disinfect shared surfaces like doorknobs, toys, and changing tables daily during outbreaks
- Avoid sharing cups, utensils, and towels with an infected person
- Teach kids to cover coughs and sneezes with their elbow
If one child in your household has HFMD, expect siblings to catch it within the incubation period (3 to 6 days). Although you can separate towels and cups, complete isolation is rarely practical in a family setting.
Common Mistakes Parents Make with HFMD Treatment
After treating hundreds of HFMD cases, these are the errors we see most often:
- Giving leftover antibiotics. HFMD is viral, so antibiotics do nothing and can cause side effects.
- Forcing food when the child refuses. Hydration matters more than calories during the acute phase. Instead, let appetite return naturally.
- Using adult oral pain gels on babies. Products containing benzocaine (like Orajel) are not safe for children under 2 because they carry serious risks.
- Rushing to the ER for the rash alone. While the blisters look concerning, unless your child shows signs of dehydration or high fever, HFMD rash resolves on its own.
- Assuming one infection means immunity. Multiple strains of the virus exist, which means your child can get HFMD more than once.
Get Your Child Checked at CityHealth
If your child’s hand foot and mouth disease treatment at home isn’t working, or you’re unsure whether symptoms warrant medical attention, walk into CityHealth Urgent Care in San Leandro. We’ll evaluate your child, rule out complications like dehydration or secondary infection, and give you a clear recovery plan.
No appointment. No long wait. Book a visit online or walk in today.




