You are 66, your knee is swollen, and you cannot wait three weeks for your primary care doctor. But before you walk into a clinic, you need to know: does urgent care take Medicare? Yes. Medicare covers urgent care visits at most clinics nationwide, including CityHealth. However, your out-of-pocket cost depends on your specific plan. Below is exactly how coverage works, what you will pay, and what to bring.
Medically reviewed by Sean Parkin, PA, CEO & Founder — Urgent Care
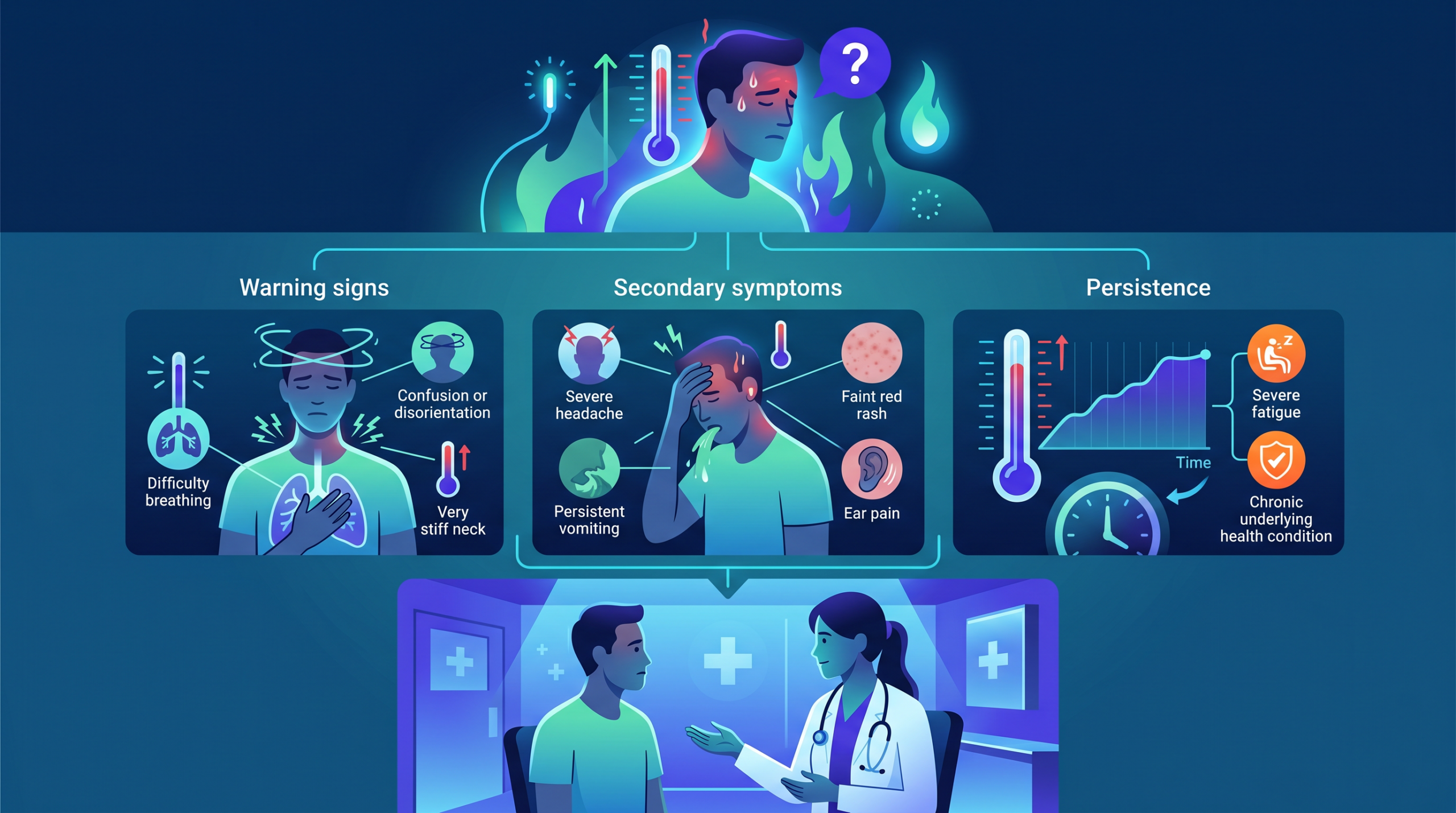
How Medicare Covers Urgent Care Visits
Medicare Part B covers outpatient care. That includes urgent care visits. When you walk into a clinic for a real medical need — an infection, a sprain, or sudden pain — Part B pays its share. According to Medicare.gov, Part B covers urgently needed care.
Here is what you pay with Original Medicare (Parts A and B):
- Part B deductible: $257 per year (2026). You pay this once before Medicare starts covering visits.
- After the deductible: Medicare pays 80% of the approved amount. You pay the remaining 20%.
- Typical urgent care visit cost: $150-$300 for the visit alone. As a result, your 20% coinsurance means $30-$60 out of pocket.
In addition, if you have a Medigap plan, it may cover some or all of that 20%. As a result, your cost could drop to zero.
Does Urgent Care Take Medicare Advantage Plans?
If you have a Medicare Advantage plan (Part C) from Humana, Aetna, or UnitedHealthcare, your costs work differently. These plans set their own copay amounts and network rules.
Most charge a flat copay for urgent care. This is typically $20-$65 per visit. In fact, that is often less than the 20% under Original Medicare.
However, your plan may have a provider network. In-network clinics cost less than out-of-network ones. Therefore, check whether the clinic takes your plan before you go. You can call ahead or look it up online.
CityHealth takes most major insurance plans, including many Medicare Advantage networks. Call (510) 984-2489 to confirm your plan before you visit.
What Services Does Medicare Cover at Urgent Care?
Medicare covers the same services at urgent care as at your regular doctor. They just need to be medically needed. For example:
- Provider evaluation and examination
- Lab work and blood tests — strep tests, flu tests, urinalysis, and basic blood panels
- X-rays — for fractures, chest conditions, and joint injuries
- Medications administered on-site — injections, nebulizer treatments, and IV fluids
- Minor procedures — wound closure, abscess drainage, and splinting
- Prescriptions — the visit itself is covered under Part B. However, medications you fill at a pharmacy are covered under Part D (your prescription drug plan)
On the other hand, Medicare does not cover routine checkups at urgent care. For instance, annual physicals and wellness visits are covered at your PCP’s office under a different benefit.
Medicare Part A vs. Part B vs. Part D: Which Pays for What?
Medicare has multiple parts. Knowing which one pays for what saves you from surprise bills:
Part A (Hospital Insurance): Covers hospital stays only. It does not apply to urgent care. However, if your visit leads to a hospital stay, Part A kicks in then.
Part B (Medical Insurance): This part pays for your urgent care visit. It covers the exam, lab work, and on-site treatments. In short, Part B is what matters when you ask “does urgent care take Medicare?”
Part D (Drug Coverage): Covers prescriptions you fill at a pharmacy. For instance, your urgent care antibiotic goes through Part D when you pick it up.
What to Bring to Urgent Care With Medicare
Walk in ready and you avoid billing issues later. Here is what to bring:
- Your red, white, and blue Medicare card (or a copy with your Medicare number)
- Medicare Advantage plan ID card (if you have Part C instead of Original Medicare)
- Medigap/supplemental insurance card (if applicable)
- Part D prescription drug card (in case you need a prescription filled)
- Photo ID
- List of current medications — names, dosages, and prescribing doctors
- List of allergies
If you forget your card, the front desk can look up your number with your Social Security number and birth date. However, having the card makes check-in much faster.
Does Medicare Cover Urgent Care When You Are Traveling?
Yes. If you travel and need urgent care with Medicare, Original Medicare works at any clinic in any state. There are no network limits with Original Medicare.
Medicare Advantage plans are different, however. Most HMO plans only cover out-of-area visits for urgent or emergency needs. In contrast, PPO plans offer out-of-network coverage at higher cost. Therefore, check your plan’s travel policy before a trip.
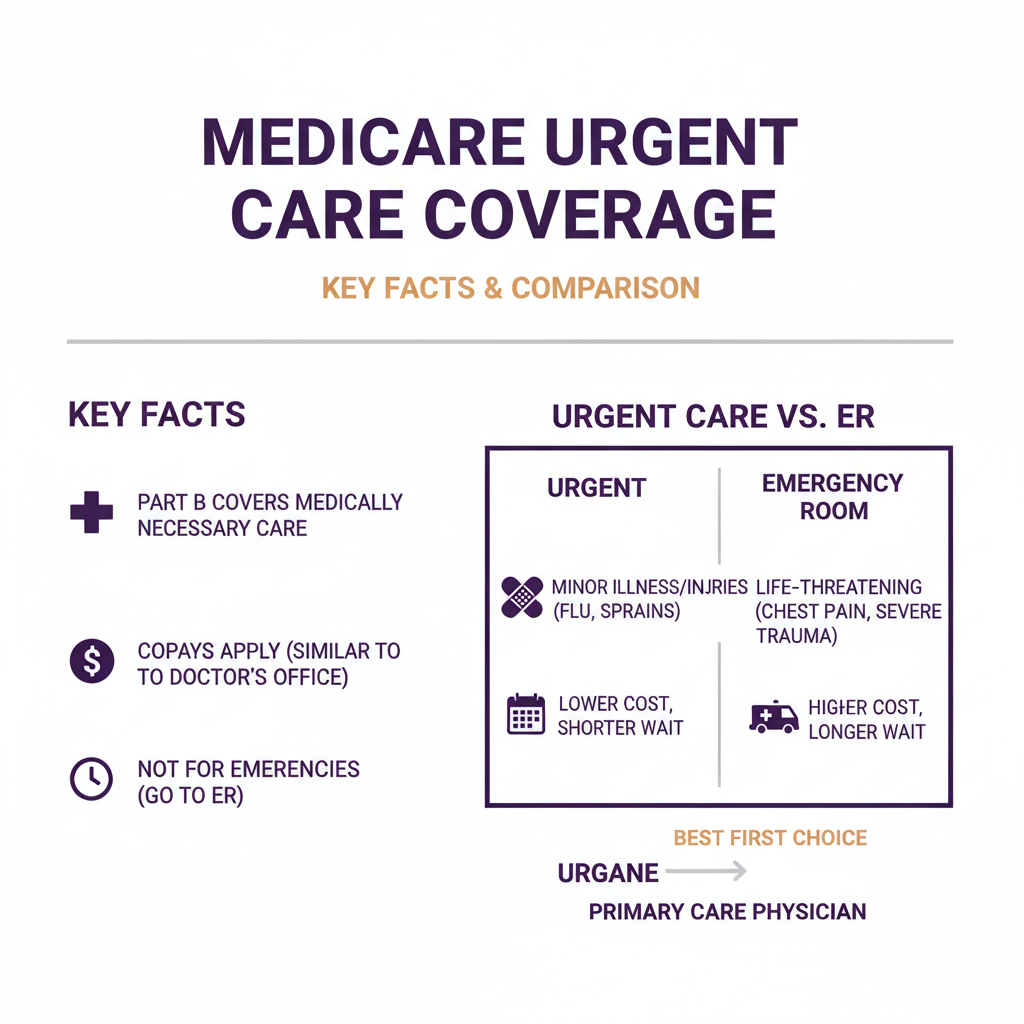
Urgent Care vs. ER: Why Medicare Patients Save at Urgent Care
For non-emergency conditions, urgent care costs significantly less than an ER visit. Furthermore, Medicare reflects that difference in what you pay:
- Urgent care visit: $150-$300 billed to Medicare. Your 20% coinsurance = $30-$60.
- ER visit (non-admitted): $500-$2,000+ billed to Medicare. Your 20% coinsurance = $100-$400+, plus potential facility fees.
Medicare does not penalize you for going to the ER. However, your wallet will feel it. If your condition is not life-threatening, urgent care gives you the same treatment for much less money.
Common Urgent Care Visits Covered by Medicare
Medicare beneficiaries visit urgent care for the same conditions as everyone else. For instance, the most common reasons include:
- Sinus infections and upper respiratory issues
- Urinary tract infections
- Back pain and joint injuries
- Skin infections, rashes, and minor lacerations
- Flu symptoms and fever
- Minor burns
- Medication refills when your PCP is unavailable
All of these are covered by Part B at urgent care. You pay your deductible and coinsurance as usual.
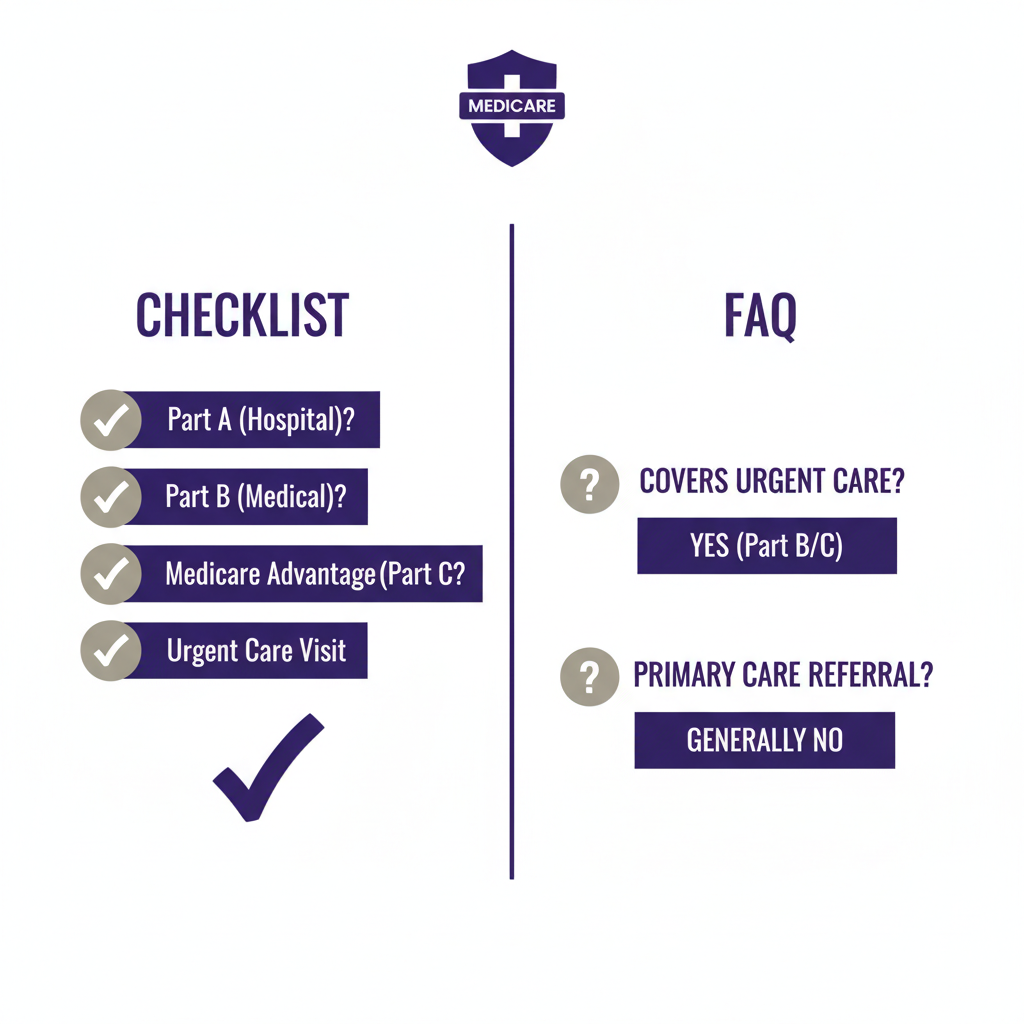

Frequently Asked Questions About Medicare at Urgent Care
Do I need a referral to go to urgent care with Medicare? No. You do not need a referral for urgent care with Original Medicare. However, some Medicare Advantage HMO plans may require one for non-urgent visits. For true urgent needs, no plan requires a referral.
Will urgent care bill me or bill Medicare directly? Most urgent care clinics bill Medicare directly. You pay your copay or coinsurance at the time of your visit. The clinic handles the rest with Medicare.
What if the urgent care center does not accept Medicare? Most do. However, if a clinic does not take Medicare, you would pay the full cost out of pocket. Therefore, call ahead to confirm before you walk in.
Can I use Medicare at any urgent care in the country? With Original Medicare, yes. Medicare Advantage plans may limit you to in-network clinics except for urgent or emergency care.
Visit CityHealth With Your Medicare Coverage Today
CityHealth accepts Medicare and most Medicare Advantage plans. In addition, you can walk in 7 days a week with no appointment and no referral needed. Our providers treat the same conditions your primary care doctor handles, and you will be seen the same day.
Visit CityHealth in San Leandro today — bring your Medicare card and get the care you need. Because urgent care does take Medicare, there is no reason to wait weeks for a PCP appointment.