Does Urgent Care Take Medicaid? What You Need to Know
Yes, urgent care does take Medicaid in most cases. However, not every clinic does. Before you walk in, one quick call can save you time and a surprise bill. This guide covers what Medicaid pays for at urgent care, how to find a clinic near you, and what to bring. If you are in California, it also covers how Medi-Cal works at CityHealth in San Leandro.
Medically reviewed by Sean Parkin, PA — CEO & Founder, CityHealth

Does Urgent Care Take Medicaid? Most Clinics Do
Most urgent care clinics in the U.S. accept Medicaid. A 2022 Urgent Care Association report found that over 70% of urgent care centers accept public insurance, including Medicaid. That number keeps growing. However, each clinic must enroll as a Medicaid provider with your state. So a clinic that takes commercial insurance may still decline Medicaid. Therefore, always call the clinic or check your state’s Medicaid directory before you go.
CityHealth in San Leandro accepts Medi-Cal, California’s Medicaid plan. Walk-in patients with Medi-Cal are seen the same day, no appointment needed.
How to Find Urgent Care That Takes Medicaid Near You
Start with your state’s Medicaid portal. Every state has an online directory where you can search for enrolled urgent care clinics by zip code. For California residents, the Medi-Cal Provider Directory is on the Department of Health Care Services website.
You can also call your Medicaid managed care plan. Most plans put a phone number on the back of your card. A rep can give you a list of in-network urgent care clinics near you in just a few minutes.
A third option: call the urgent care clinic before you leave home. Ask two things — “Do you take Medicaid?” and “Do you take my specific plan?” Because plans like Molina, Anthem, and Health Net each need separate clinic enrollment, a clinic may take Medicaid broadly but not your specific plan. For more on how urgent care accepts insurance across plan types, that resource covers both public and private coverage.
What Does Medicaid Cover at Urgent Care?
Medicaid covers a wide range of services at enrolled urgent care clinics. Coverage follows federal standards set by the Centers for Medicare and Medicaid Services (CMS). As a result, most members get access to the services below.
Sick Visits and Exams
Medicaid covers sick visits for things like strep throat, urinary tract infections, colds, skin infections, and minor cuts. Your cost is typically $0 to $4, depending on your state. In addition, many states waive copays entirely for low-income members. To see the full list of conditions urgent care treats, that resource covers everything from injuries to women’s health.
Lab Work and Testing
Most states cover lab tests at no cost when the clinic runs them on-site. These include strep tests, flu swabs, urine tests, and blood draws. However, if the clinic sends samples to an outside lab, that lab must also be enrolled in Medicaid. Ask the front desk before agreeing to outside testing.
X-Rays and Imaging
Medicaid covers X-rays and imaging when they are medically needed. For example, chest X-rays for suspected pneumonia, arm or leg X-rays for possible fractures, and sinus films are all covered. Coverage applies when the clinic bills Medicaid directly. In addition, if you get referred to a separate imaging center, verify they take Medicaid before you go.

Does Urgent Care Take Medicaid for Physicals?
Yes, many urgent care clinics do physicals for Medicaid members. This includes school physicals, sports physicals, employment physicals, and adult wellness exams. Coverage depends on how the visit is billed and your state’s rules. However, most enrolled clinics can bill for these visits directly.
Children on Medicaid get physicals through the EPSDT benefit (Early and Periodic Screening, Diagnostic, and Treatment). This federal rule requires states to cover well-child visits at no cost. So if the clinic is an enrolled EPSDT provider, your child’s physical is covered. If the physical includes lab work — like a blood test or TB skin test — that is usually covered too.
Does Urgent Care Take Medicaid for Kids?
Yes. Children on Medicaid can get care at any enrolled urgent care clinic. Covered services include sick visits, well-child exams, shots, ear infections, rashes, and minor injuries. Because children make up about 40% of all Medicaid members, most urgent care clinics actively accept pediatric Medicaid. However, some managed care plans ask for a referral from a primary care provider. So check your plan’s rules before you go.
Medicaid vs. Medicare at Urgent Care
Medicaid and Medicare are two separate programs. Medicaid covers low-income people of any age. Medicare covers adults 65 and older plus some disabled adults. Some people have both — this is called dual eligibility. For those patients, Medicare pays first and Medicaid covers what is left.
At urgent care, Medicare Part B covers office visits, labs, and imaging. Your share is typically 20% of the Medicare-approved amount after your deductible. Medicaid copays, by contrast, are usually $4 or less. For a full breakdown of urgent care copay costs by plan type, that guide compares what patients pay under various plans.
Also note that clinics must enroll in Medicare and Medicaid separately. Therefore, a clinic may take one program but not the other. Always confirm both when you call.
Can You Use Out-of-State Medicaid at Urgent Care?
Medicaid covers you in your home state. If you travel, your plan covers true emergencies — conditions that could cause serious harm if not treated right away. However, routine urgent care visits like a sinus infection are usually not covered out of state.
Federal law requires all Medicaid programs to cover emergency care when you travel. The test is whether a reasonable person would believe they needed immediate care. If yes, coverage applies. Still, if you have moved recently, contact your old state’s Medicaid office to update your address. Until your new state enrollment is active, your coverage stays with your original state.
What to Bring to Urgent Care With Medicaid
Arriving prepared speeds up registration and cuts down on billing errors. Bring these items:
- Your Medicaid card — physical card or screenshot from your state’s Medicaid app
- A photo ID — driver’s license, state ID, or passport
- Your managed care plan card — if your Medicaid runs through Molina, Anthem, or Health Net
- A list of your current medications — include dosages and prescribing providers
- Your primary care provider’s name and phone — some plans need care coordination
- A referral number — only if your plan requires referrals for urgent care
If your Medicaid card has not arrived yet, ask your state Medicaid office for a temporary proof of coverage letter. Most clinics accept this at check-in while your card is on the way.
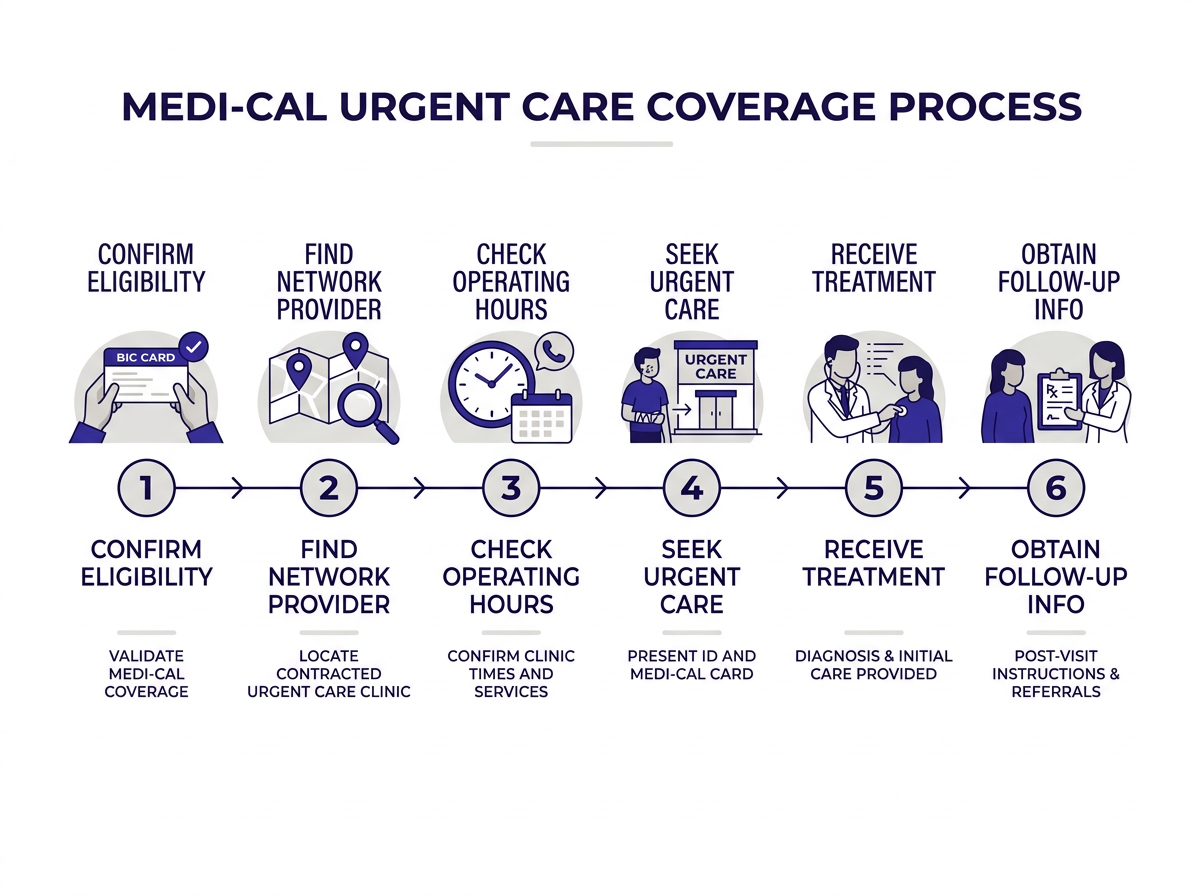
CityHealth in San Leandro accepts Medi-Cal.
Walk in at 201 Dolores Ave, San Leandro, CA 94577 — no appointment needed. Mon 10am–7pm, Tue–Fri 9am–7pm, Sat–Sun 9am–5pm.
CityHealth San Leandro Accepts Medi-Cal
CityHealth is a walk-in urgent care clinic in San Leandro, California. We accept Medi-Cal. Walk-in patients are seen the same day with no appointment needed. Services include sick visits, labs, X-rays, physicals, and more — all covered under Medi-Cal for eligible patients. Call us with your plan name before your visit to confirm your specific coverage.
Frequently Asked Questions
- Can I use Medicaid at any urgent care?
- No. Each urgent care clinic must enroll as a Medicaid provider. Always call ahead or check your state’s Medicaid directory to confirm the clinic takes your plan.
- Does Medicaid cover urgent care visits fully?
- In most cases, yes. Medicaid covers the full cost of urgent care visits with little to no copay. Details vary by state and plan.
- Does urgent care take Medi-Cal in California?
- Yes, many urgent care clinics in California accept Medi-Cal, including CityHealth in San Leandro. Call ahead to confirm your specific plan is accepted.