Child Hand Foot and Mouth Disease: Symptoms, Duration, and When to Walk In
When a child hand foot and mouth infection first strikes, it can be alarming — especially if you’ve never seen it before. Your child woke up with a fever and won’t touch their breakfast. By afternoon, they’re drooling and crying every time they try to swallow. Then you notice small blisters forming on their palms. In fact, this illness is one of the most common childhood illnesses, and one of the most alarming to see for the first time.
The good news is that most children recover fully within 7 to 10 days. However, knowing what to watch for — and when to seek care — makes all the difference.
Medically reviewed by Susana Quezada, NP — Nurse Practitioner, CityHealth

What Is Child Hand Foot and Mouth Disease?
Child hand foot and mouth disease (HFMD) is a viral illness. It primarily affects children under 5 years old, though older kids and adults can get it too. The most common cause is Coxsackievirus A16. Another strain, Enterovirus 71, also causes HFMD — and it can lead to more serious complications in some cases.
Neither virus has an antiviral treatment. Consequently, there’s no prescription that makes it go away faster. Instead, treatment focuses on managing symptoms and keeping your child comfortable while their immune system does the work.
According to the CDC, HFMD is most common in summer and fall. Notably, outbreaks frequently spread through daycares and preschools, where young children are in close contact throughout the day.
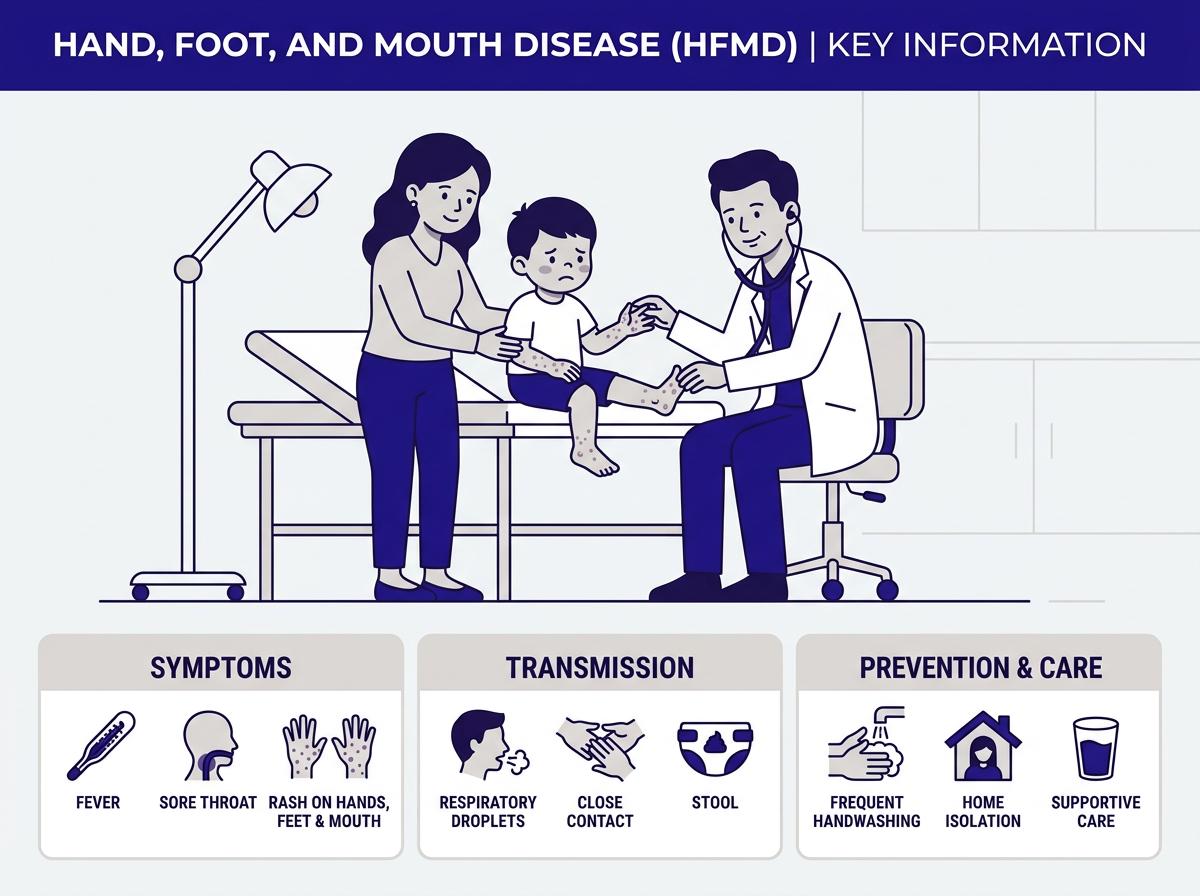
Symptoms to Watch For
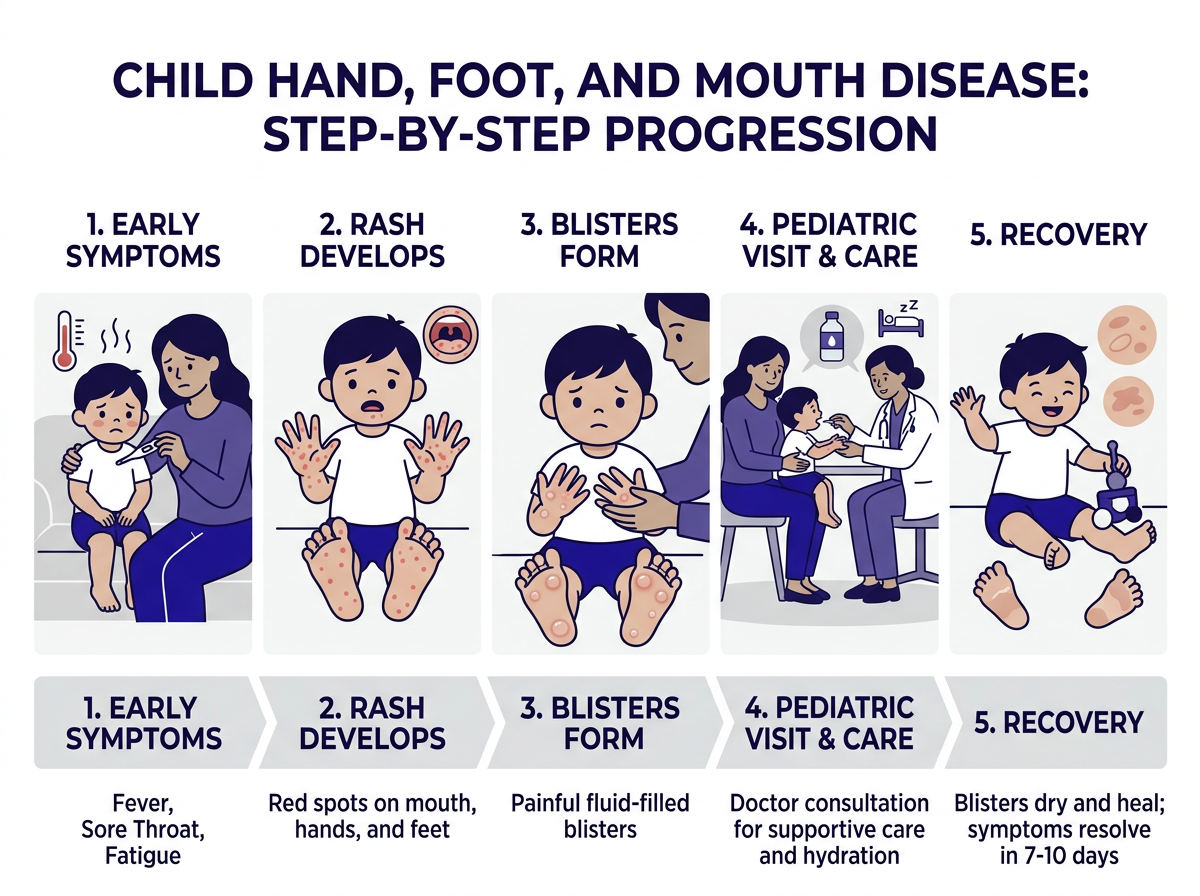
This viral illness doesn’t show all its symptoms at once. Instead, it follows a predictable pattern over several days. Knowing the stages helps you recognize it early.
Stage 1 — Fever: The illness usually starts with a fever between 101°F and 103°F. Your child may also seem tired, lose their appetite, or complain of a sore throat. This early phase lasts one to two days.
Stage 2 — Mouth sores: After the fever begins, painful sores appear inside the mouth. They start as small red spots, then quickly turn into ulcers. Specifically, you’ll find them on the tongue, inner cheeks, and gums. These sores are often what stops children from eating or drinking — they hurt.
Stage 3 — Skin rash and blisters: Within one to two days of the mouth sores, a rash develops. It appears as small red spots or fluid-filled blisters on the palms of the hands, the soles of the feet, and sometimes the buttocks or genitalia. Unlike chickenpox, the rash from HFMD is usually not itchy.
Not every child develops all three stages. Some may only have mouth sores. Others may get the rash without much fever. Regardless, the combination of fever, mouth ulcers, and blisters on the hands and feet is the hallmark of this illness.
How Long Does Child Hand Foot and Mouth Last?
In most cases, children recover from this infection within 7 to 10 days. The fever typically resolves within the first three days. Mouth sores often heal within a week. Additionally, the skin blisters dry out and crust over as the illness clears.
The incubation period — the time between exposure and the first symptoms — is typically 3 to 6 days. For example, if your child was exposed at daycare on Monday, symptoms may not appear until Thursday or Sunday.
Even after symptoms resolve, your child can still carry and shed the virus for several weeks. Notably, most daycares and schools require children to stay home until they are fever-free and their sores are crusted or healing. Therefore, check with your child’s facility for their specific policy.
How Does Child Hand Foot and Mouth Disease Spread?
In fact, the disease is highly contagious. It spreads through several routes, which is why it moves so quickly through daycares and preschools.
- Fecal-oral contact: The virus lives in the stool. It spreads when contaminated hands touch the mouth — a common occurrence with toddlers.
- Respiratory droplets: Coughing and sneezing release the virus into the air and onto surfaces.
- Blister fluid: Direct contact with fluid from the blisters can transmit the virus to another person.
- Contaminated surfaces: The virus can survive on toys, doorknobs, and changing tables.
Children with hand foot and mouth disease are most contagious during the first week of symptoms. However, they can continue shedding the virus for weeks afterward — even without symptoms. Given that, frequent handwashing is the single most effective way to limit spread.
Home Care for HFMD
There’s no shortcut to recovery from HFMD. However, the right home care makes your child more comfortable and helps prevent complications.
Keep fluids flowing. This is the top priority. For example, the mouth sores make swallowing painful, so many children resist drinking. Offer cold water, ice chips, diluted apple juice, or cold milk frequently throughout the day. Popsicles and cold smoothies can be easier to tolerate than warm liquids.
Choose soft, bland foods. Avoid anything acidic, salty, or spicy — these will aggravate mouth sores. Instead, try yogurt, applesauce, mashed potatoes, or cold oatmeal. Small, frequent offerings work better than large meals.
Use a fever reducer if needed. Acetaminophen (Tylenol) or ibuprofen (for children over 6 months) can help bring down fever and ease discomfort from these symptoms. Always follow dosing instructions for your child’s weight and age. Additionally, never give aspirin to children.
Apply cool compresses. A cool, damp cloth on the forehead or blistered areas can offer temporary relief. Moreover, cool baths may also help reduce fever and soothe irritated skin.
Let them rest. Their immune system is working hard. Since rest helps the body fight the virus, keep your child home from school or daycare — not just because they’re contagious, but because they need the downtime to heal.
Warning Signs That Need Urgent Care
In most cases, the condition resolves at home. But some situations call for a same-day evaluation. Watch for these warning signs closely.
Dehydration is the most serious complication of this illness. The mouth sores make drinking painful, which puts young children at real risk. Therefore, learn to recognize the signs of dehydration: dry mouth, no tears when crying, fewer wet diapers than usual, sunken eyes, or unusual drowsiness. If you notice any of these, don’t wait.
Fever above 104°F warrants same-day evaluation. While fever is a normal part of HFMD, a very high fever may indicate a secondary infection or a more severe viral strain. You can read more about monitoring your child’s fever and when it becomes a concern.
Not drinking for 8 or more hours is a red flag, especially in toddlers and infants. Even if your child isn’t dehydrated yet, this level of fluid refusal puts them at risk quickly. Therefore, act early rather than waiting to see if it resolves on its own.
Severe headache, neck stiffness, or unusual confusion are rare but serious signs. In uncommon cases — particularly with Enterovirus 71 — the infection can affect the nervous system. Importantly, these symptoms require immediate evaluation.
Worsening symptoms after day 5 are also worth a visit. The illness should start improving within a week. As a result, if your child is getting worse — not better — it’s time to be seen.
Can Urgent Care Help with Child Hand Foot and Mouth Disease?
Yes — and in many cases, it’s the right call. Furthermore, you don’t need to wait days for a pediatrician appointment when your child is miserable and you’re not sure what you’re dealing with.
At walk-in urgent care, a provider can confirm the diagnosis, rule out other causes of fever and rash, assess your child’s hydration status, and advise you on what to do next. Additionally, if there’s a secondary infection — like a bacterial skin infection on top of the blisters — that can be identified and treated right away.
Urgent care is also appropriate when you just need a professional set of eyes. Essentially, parenting a sick toddler is stressful. Above all, you shouldn’t have to guess whether your child is okay.
CityHealth in San Leandro sees children and adults for conditions like HFMD — no appointment required. Our team can confirm the diagnosis, check for complications, and give you a clear plan for home care and when to return.
If your child has signs of dehydration, a fever over 104°F, or you’re just not sure whether it’s child hand foot and mouth disease — walk in to CityHealth in San Leandro. No appointment needed. We see children and adults, same day. Book a visit or walk right in.



